Dr. Ivar Mendez met with Federal Health Minister Jane Philpott earlier this year to talk about robotic technology. Photo courtesy @janephilpott, Twitter.
An expert in remote healthcare says a new robotic machine is a gamechanger for northern Saskatchewan mothers-to-be, who face higher rates of infant mortality than the rest of the province.
Dr. Ivar Mendez is part of a team that’s testing out a tele-robotic ultrasound system called MELODY, purchased last year through a generous donation by the Leslie and Irene Dubé Foundation to the Royal University Hospital (RUH) in Saskatoon. The MELODY system’s final destination will be decided in the fall, and so far it has been used in Pelican Narrows and La Loche on a trial basis.
MELODY allows a nurse in a remote community to operate the ultrasound’s probes while a specialist at RUH communicates by video and instructs their motions in order to perform a real-time assessment, diagnosis and patient management. The initial studies found this method to be just as accurate and safe as a traditional ultrasound system, said Mendez, who is the Head of the Department of Surgery at the University of Saskatchewan and Saskatoon Health Region.
In Mendez’s view, pregnant women and their unborn babies will benefit most from this new technology because of the young population in the north: he says over 60 per cent of many communities are made up of children under 15. Currently, he says, women in remote northern communities can face prohibitive travel times to Saskatoon or Regina for pre-natal ultrasounds because of the limited number of ultrasounds and technicians in the north.
“If you have to travel two or three days to get an ultrasound, some young mothers do not do that because of issues that they have to contain at home; (they) don’t have the time, don’t have the resources to have a pre-natal ultrasound. And many will need more than one ultrasound. So that is a big problem, the access to pre-natal ultrasound in northern communities,” he said.
“That’s why morbidity and mortality for mothers and newborns is higher in northern communities.”
While an ultrasound can also be used on abdominal conditions like a gallbladder issue, pre-natal ultrasounds are a priority for Mendez because “we need to provide mothers, especially in Indigenous communities, with free access and easy acces to pre-natal ultrasounds.”
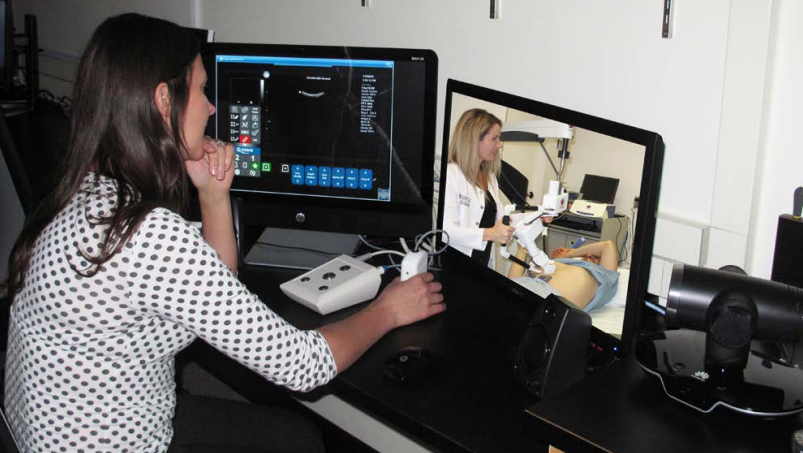
A sample of what a doctor would see at RUH, with the video screen showing what’s happening at the remote location. Photo courtesy RUH Foundation’s 2016-17 report.
For Mendez, who pioneered the use of the “doctor in a box” and Rosie the robot — a self-wheeling machine with a human-height monitor that allows a doctor to appear remotely from another community while monitoring vitals and visually assessing a patient by video — in northern Saskatchewan, the MELODY system is another step towards improving healthcare in the north.
“As Canadians we think that healthcare is the same for everybody, and you and I know that that’s not true because access to healthcare is different if you live in Saskatoon than if you in Buffalo River. So the idea is, can we use technology to bridge that gap? Can we make things more accessible to people that need the most? That is really my philosophy. That is my passion,” he said.
So far, there are about six Rosie the robots deployed across the north, and can be easily shipped for use in different communities. A late 2016 study in Pelican Narrows found that 63 per cent of kids who were remotely seen by an intensivist in Saskatoon were able to safely be assessed and treated in their own community thanks to the use of Rosie’s remote technology.
“That’s a huge thing because you can treat the problem in their own community so the kid can sleep in his or her own bed and doesn’t need to have an unnecessary trip to Saskatoon to be taken care of,” Mendez said.
The MELODY system is less mobile than the other remote technologies, meaning it will stay in one location permanently. While Mendez hopes to see more put in place in the future, currently there is only one in the province. Regardless, he sees a lot of potential.
“For the first time, you will be able to have the ultrasound in your own community and if there’s any issues that have to do with potential complications at the time of childbirth you will be able to be referred with time,” he said.
He expects to see safer in-community baby deliveries as well.
“I think that’s an important thing for the communities to have your baby not in a distant location, but where your family is.”
Mendez said Saskatchewan is the most advanced province when it comes to using what he calls “remote presence technologies,” which led a recent delegation from Australia and New Zealand to visit the province. He said other provinces are also looking to Saskatchewan for guidance on remote healthcare.
